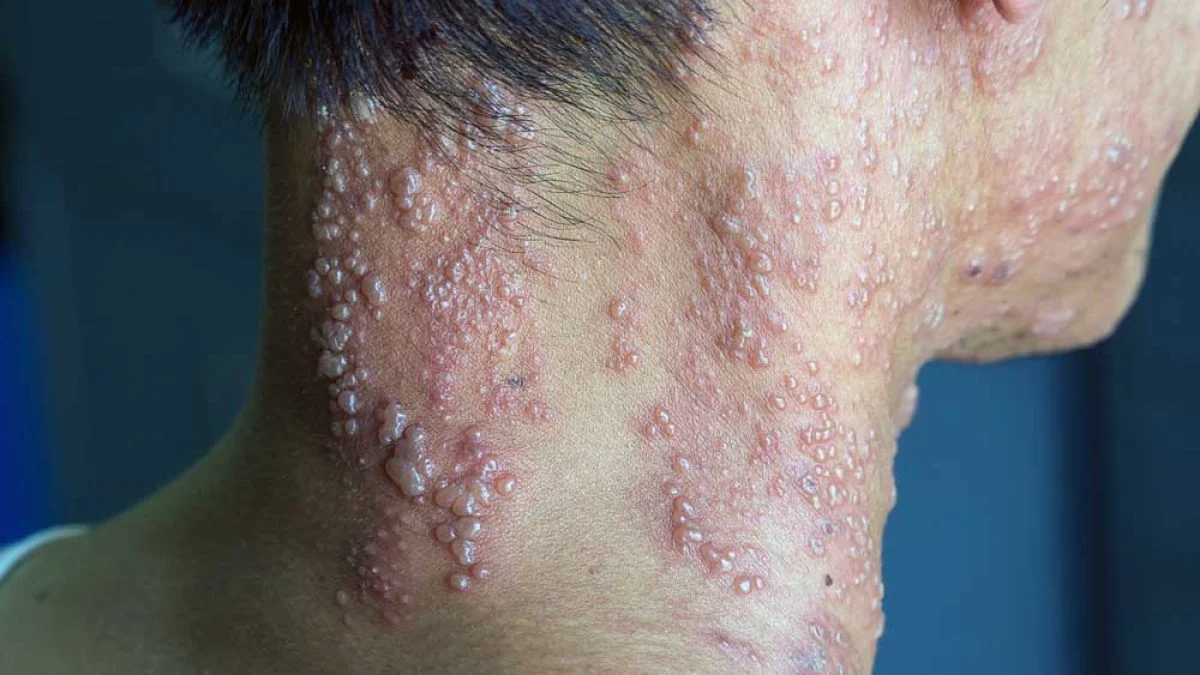
Herpes Zoster Treatment
What is Herpes Zoster? Herpes zoster, commonly known as shingles, is a viral infection caused by the reactivation of the varicella-zoster virus - the same virus that causes chicken pox. After a person recovers from chicken pox, the virus remains dormant (inactive) in nerve tissues near the spinal cord and brain. Years or decades later, the virus can reactivate, traveling along nerve pathways to the skin and causing a painful, blistering rash. At Ojas Clinic, we provide comprehensive care to manage symptoms, speed healing, and prevent complications like post-herpetic neuralgia.
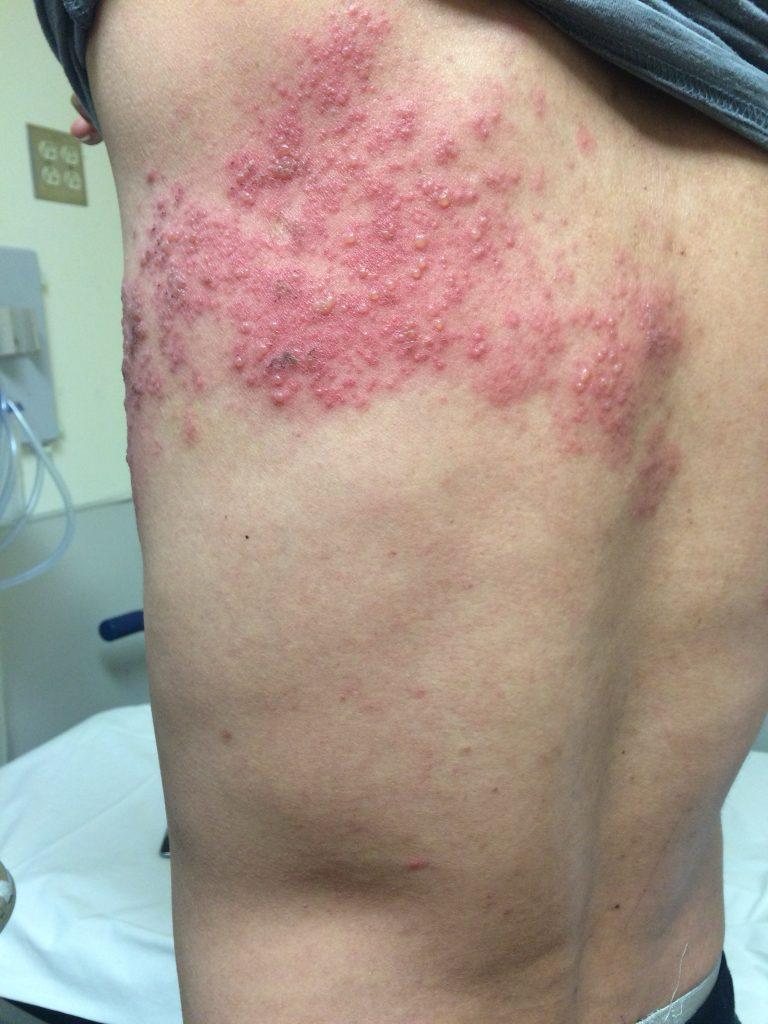
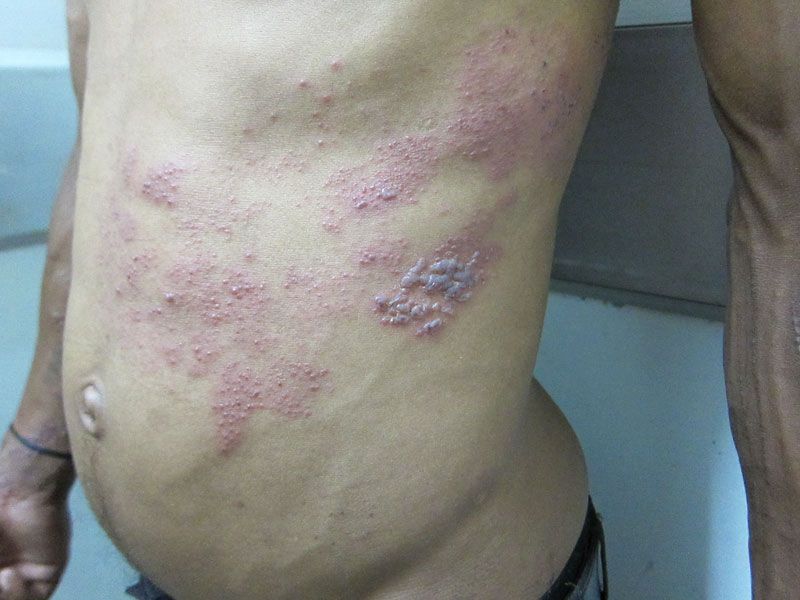
Dermatome Distribution
Shingles typically affects one side of the body along a specific dermatome (area of skin supplied by a single nerve). The most common locations include:
The rash rarely crosses the midline of the body - this is a key diagnostic feature.
Our Treatment Approach
Antiviral Medications
Antiviral drugs are most effective when started within 72 hours of rash onset. They help:
- Reduce severity and duration of symptoms
- Speed up healing of blisters
- Lower the risk of post-herpetic neuralgia
- Reduce viral shedding
Pain Management
- Over-the-counter pain relievers: Acetaminophen, ibuprofen
- Prescription pain medications: For severe pain
- Topical treatments: Lidocaine patches, capsaicin cream
- Nerve blocks: For severe or persistent pain
Home Care & Symptom Relief
- Cool compresses on blisters to soothe pain
- Cool baths
- Loose, soft, breathable clothing
- Keep the rash clean and dry
- Calamine lotion for itching (after blisters crust)
- Rest and stress reduction
Why Choose Ojas for Herpes Zoster?
At Ojas Skin & Hair Clinic, we provide specialized care for shingles patients:
- Expert Dermatologists: Specialized in viral skin infections and nerve pain management
- Early Intervention: Prompt treatment within the critical 72-hour window
- Comprehensive Pain Management: Multimodal approach to acute and chronic pain
- Post-Herpetic Neuralgia Care: Specialized treatment for persistent nerve pain
- Ophthalmic Shingles Management: Coordination with eye specialists when needed
- Personalized Care: Treatment plans tailored to your age and health status
- Follow-up Support: Long-term monitoring for complications
We understand that shingles can be extremely painful and distressing. Our team is committed to providing compassionate care that addresses both your immediate symptoms and long-term recovery.
Frequently Asked Questions
Shingles itself is not contagious. However, the varicella-zoster virus can be transmitted from a person with active shingles to someone who has never had chicken pox. This person would then develop chicken pox, not shingles. Transmission occurs through direct contact with the fluid from blisters. Once blisters have crusted over, the person is no longer contagious. People with shingles should keep the rash covered and avoid contact with pregnant women, newborns, and immunocompromised individuals.
The active phase of shingles typically lasts 2-4 weeks. The timeline includes: prodromal phase (1-5 days of pain/tingling before rash), blister formation (3-5 days), blister crusting (7-10 days), and healing (2-4 weeks). However, pain can persist longer as post-herpetic neuralgia in some patients. Early antiviral treatment can significantly shorten the duration and severity of the illness.
Yes, it is possible to get shingles more than once, though it's not common. Recurrence rates are about 1-6% in immunocompetent individuals. The risk of recurrence is higher in people with weakened immune systems. The shingles vaccine can significantly reduce the risk of both first-time and recurrent shingles, which is why vaccination is recommended even for those who have had shingles before.
Post-herpetic neuralgia (PHN) is persistent nerve pain that continues after the shingles rash has healed. It's the most common complication of shingles, affecting about 10-18% of patients. The pain can be severe and debilitating - described as burning, stabbing, or shooting. PHN can last for months or even years. Risk increases with age, and early antiviral treatment can reduce the risk. At Ojas Clinic, we offer specialized treatments for PHN including nerve pain medications, nerve blocks, and topical therapies.
Yes, shingles can affect the eye (herpes zoster ophthalmicus) when the virus involves the ophthalmic branch of the trigeminal nerve. This is a medical emergency that requires immediate attention. Symptoms include rash on the forehead, nose, or around the eye, eye redness, swelling, pain, and vision changes. Without prompt treatment, it can lead to corneal damage, glaucoma, and permanent vision loss. If you have shingles near your eye, seek medical attention immediately.
Yes, stress is a well-known trigger for shingles reactivation. Physical or emotional stress can weaken the immune system, allowing the dormant varicella-zoster virus to reactivate. Other triggers include illness, surgery, trauma, and certain medications. While you can't always prevent stress, managing stress through relaxation techniques, adequate sleep, exercise, and a healthy lifestyle may help reduce your risk. If you're under significant stress and concerned about shingles, ask about vaccination options.